Why Calf Pain Shouldn’t Be Ignored
Calf muscle pain can stop you right in your tracks—whether you’re running through Maybury State Park, chasing after your kids, or simply walking to your car after a long workday. That sharp twinge or dull ache in the back of your lower leg affects athletes and everyday people alike, and it’s often a signal that something needs attention.
Quick Answer: What You Need to Know About Calf Muscle Pain
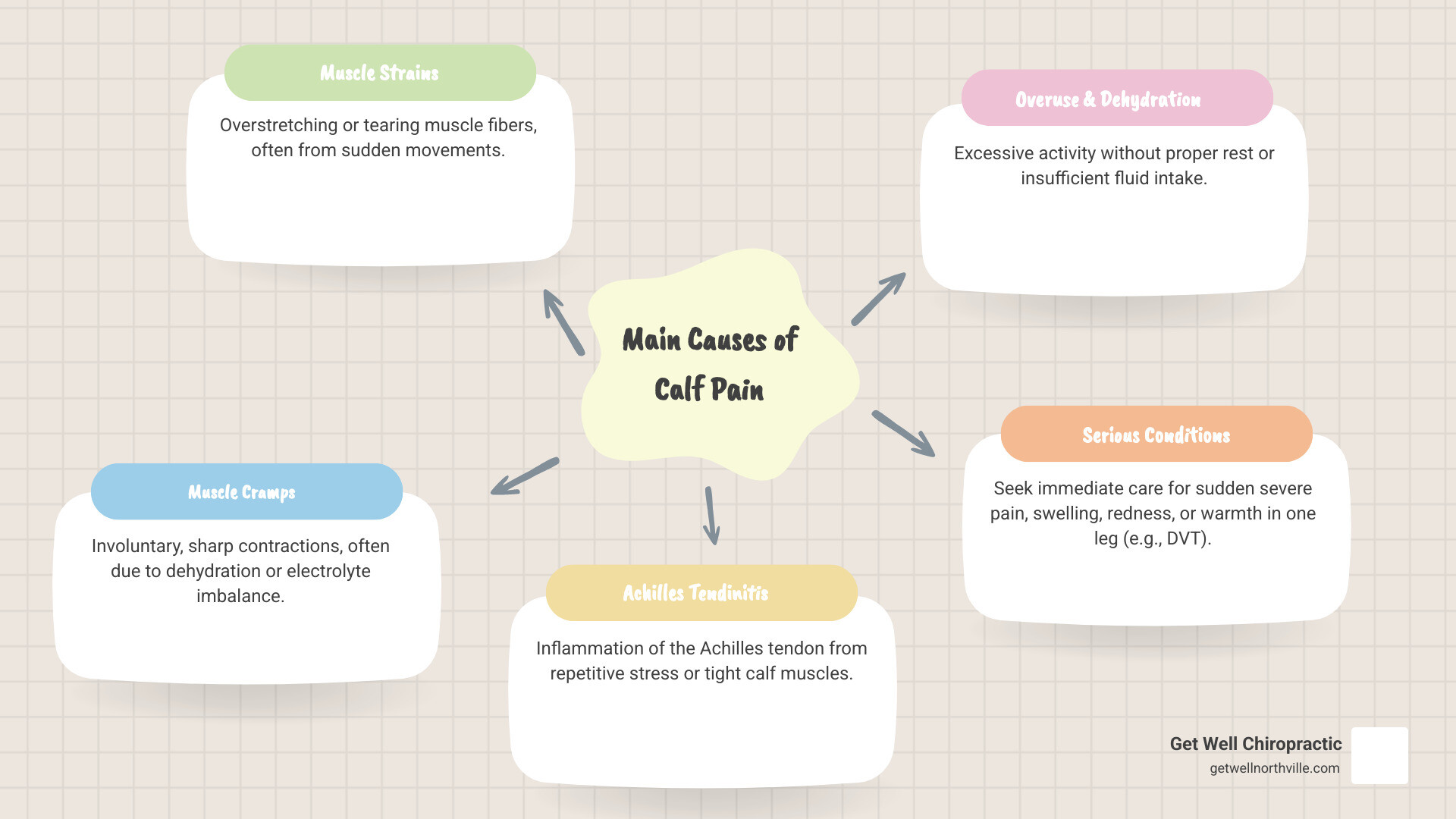
- Most Common Causes: Muscle strains, cramps (charley horses), Achilles tendinitis, overuse, or dehydration
- Immediate Treatment: RICE method (Rest, Ice, Compression, Elevation) for mild injuries
- Recovery Time: 10-12 days for mild strains, 16-21 days for moderate strains, up to 6 months for severe tears
- Seek Emergency Care If: You have sudden severe pain with swelling, redness, or warmth in one leg (possible DVT—up to 10% of calf pain cases), chest pain, or difficulty breathing
- Prevention: Proper warm-ups, stretching, gradual exercise progression, and staying hydrated
Your calf muscles—the gastrocnemius and soleus—do more than you might realize. They’re essential for walking, running, jumping, and even just standing up from a chair. When they hurt, your whole life can feel limited.
The good news? Most calf pain responds well to simple treatments, and understanding what’s causing your discomfort is the first step toward getting back to the activities you love. Whether it’s a minor strain that needs rest or something more serious requiring professional attention, this guide will help you understand what’s happening in your lower leg and what to do about it.
Research shows that while most people recover fully from pulled calf muscles without permanent damage, knowing when to seek help can make all the difference—especially since serious conditions like deep vein thrombosis can sometimes masquerade as simple muscle pain.
Understanding Your Calves: The Foundation of Your Lower Leg
Our calves are truly unsung heroes of our mobility. Located at the back of your lower leg, these powerful muscles are crucial for nearly every movement involving your feet and ankles. Understanding their anatomy and function is the first step in appreciating their importance and protecting them from injury.
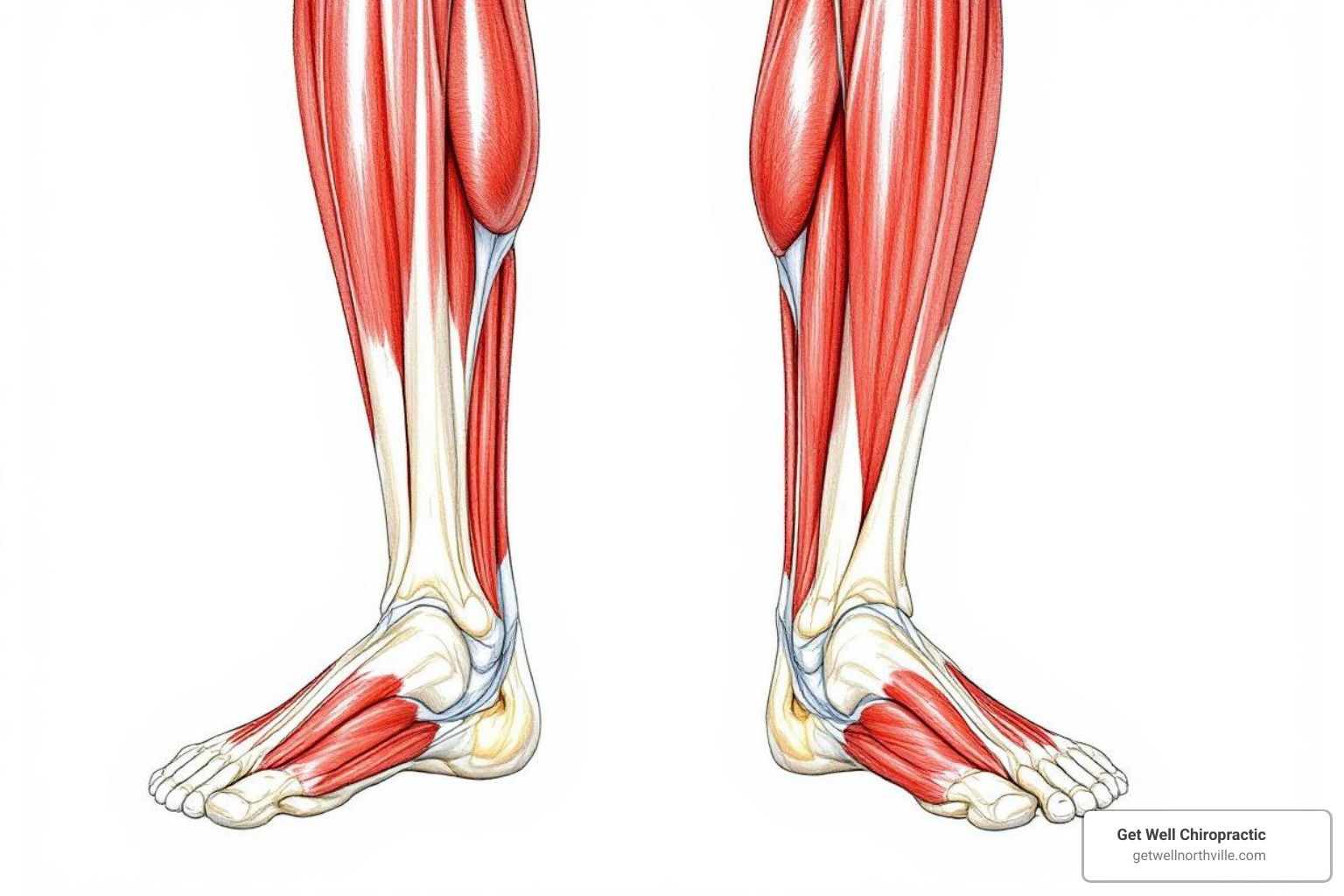
The calf is primarily composed of two main muscles:
- Gastrocnemius muscle: This is the larger, more superficial muscle that gives the calf its distinct shape. It crosses both the knee and ankle joints, playing a key role in knee flexion and plantarflexion (pointing your toes down). It’s particularly active during powerful, explosive movements like jumping, sprinting, and pushing off the ground.
- Soleus muscle: Lying underneath the gastrocnemius, the soleus is a broad, flat muscle that primarily affects the ankle joint. It’s essential for prolonged standing and walking, providing endurance and stability.
Both the gastrocnemius and soleus muscles merge at the bottom of the calf to form the Achilles tendon, the strongest and thickest tendon in the body. This tendon then attaches to your heel bone (calcaneus). Together, this muscle-tendon unit allows us to:
- Walk and Run: Propelling us forward with each step.
- Jump: Providing the explosive power needed to leave the ground.
- Flex the foot: Enabling movements like standing on our tiptoes.
When these muscles are healthy, we can enjoy all the wonderful activities Michigan has to offer, from a leisurely stroll in Northville to a more intense workout. When they’re not, even simple tasks can become a painful challenge.
Common Causes of Calf Muscle Pain
Calf muscle pain can manifest in many ways, from a sudden, sharp sensation to a persistent, dull ache. Often, the cause is a straightforward muscle issue like a strain or a cramp. Let’s explore some of the most frequent culprits that can make your calves protest.
Calf Muscle Strains (Pulled Calf Muscle)
A calf muscle strain, often called a “pulled calf muscle,” occurs when the muscle fibers in your calf are overstretched or torn. This can range from microscopic tears (mild strain) to a complete rupture of the muscle (severe strain).
- What causes it? Strains typically happen during sudden movements, such as accelerating quickly, jumping, or making abrupt stops. Activities like tennis, basketball, or running are common triggers. Sometimes, it’s referred to as “tennis leg” because the gastrocnemius muscle is frequently injured during explosive pushes off the foot.
- Symptoms: You might experience a sudden, sharp pain at the back of your lower leg, making it difficult to put weight on the affected leg or stand on your toes. Other symptoms include:
- Bruising on the calf muscle
- Swelling in the calf area
- Tenderness to the touch
- Difficulty tensing your calf muscles
- A snapping or popping sensation at the moment of injury
- Muscle pain when flexing your ankle or pointing your toes
Most people with a strained calf muscle can’t continue their activity immediately after the injury. For more detailed information on preventing and rehabilitating calf strains, you can refer to a guide on calf strains from Sports Medicine Australia.
Muscle Cramps (Charley Horse)
Picture this: you’re enjoying a peaceful night’s sleep, or perhaps finishing up a workout, and suddenly, your calf muscle seizes up in an intense, involuntary contraction. This is a muscle cramp, commonly known as a “charley horse.”
- What causes it? While the exact mechanism can be complex, common causes include:
- Dehydration: Not drinking enough water, especially during or after physical activity.
- Electrolyte imbalance: A loss of essential minerals like potassium, sodium, calcium, or magnesium through sweating.
- Muscle overuse or overexertion: Pushing your muscles too hard without adequate rest.
- Lack of stretching: Tight muscles can be more prone to cramping.
- Weak muscles: Muscles that aren’t conditioned for the activity being performed.
- Symptoms: The primary symptom is a sudden, sharp, often excruciating pain in the calf, accompanied by a visible or palpable hardening of the muscle. The cramp usually lasts from a few seconds to several minutes.
- Treatment: When a cramp strikes, try to gently stretch the affected muscle. Massaging the calf can also help to relax the muscle fibers. Applying a warm towel or heating pad can also provide relief. Staying well-hydrated and ensuring you have adequate electrolyte intake are key preventive measures.
Achilles Tendinitis
Our Achilles tendon is a marvel of engineering, connecting our powerful calf muscles to our heel bone. But like any hard-working structure, it can become inflamed, leading to Achilles tendinitis.
- What causes it? This condition typically arises from repetitive stress or overuse, often seen in runners or individuals who suddenly increase the intensity or duration of their physical activity. Tight calf muscles can also put extra strain on the Achilles tendon, increasing the risk of inflammation.
- Symptoms: Common signs include:
- Morning stiffness and tenderness in the Achilles tendon, which may improve with activity.
- Pain along the back of the leg, just above the heel.
- Pain that worsens with activity, especially running or jumping.
- Thickening of the tendon.
- Swelling in the area.
If left unaddressed, Achilles tendinitis can become chronic or even lead to a more serious Achilles tendon rupture, so it’s wise to pay attention to these early warning signs.
When Calf Pain Signals Something More Serious
While muscle strains and cramps are common and often resolve with home care, it’s crucial to understand that calf muscle pain can sometimes be a symptom of more serious underlying medical conditions. Knowing the “red flags” can be life-saving.
Red Flags: When to Seek Immediate Medical Attention
Some conditions require prompt medical evaluation to prevent serious complications. If you experience any of the following, please seek immediate medical attention:
- Deep Vein Thrombosis (DVT): This is a blood clot that forms in a deep vein, usually in the leg. DVT is a medical emergency because the clot can break loose and travel to your lungs, causing a pulmonary embolism, which can be fatal.
- Symptoms: DVT often presents with calf muscle pain that may worsen when standing or walking. Crucially, look for:
- Sudden, unexplained swelling in one leg (this is a key differentiator from muscle strain).
- Redness or discolored skin on the leg.
- Warmth to the touch in the affected calf.
- Severe pain that doesn’t seem to improve.
- According to research, up to 10% of people with symptoms of calf pulls actually have DVT, making it a critical condition to rule out.
- If you suspect DVT, contact your doctor right away or head to the nearest emergency room. You can find more information about DVT from Cleveland Clinic.
- Symptoms: DVT often presents with calf muscle pain that may worsen when standing or walking. Crucially, look for:
- Sudden, extreme leg swelling.
- Calf pain accompanied by fever over 100°F.
- A pale or cool swollen leg.
- Chest pain or trouble breathing, especially if combined with leg pain, could indicate a pulmonary embolism. In this case, call emergency services (911) immediately.
Other Conditions That Can Cause Calf Pain
Beyond DVT, several other conditions can cause calf muscle pain that aren’t directly related to a muscle injury:
- Sciatica: This refers to pain radiating along the path of the sciatic nerve, which branches from your lower back through your hips and buttocks and down each leg. If the nerve is pinched or irritated in your lower back, it can cause burning, tingling, numbness, or weakness that extends into your calf. The pain might come and go or be constant.
- Neurogenic Claudication: This condition is often caused by spinal stenosis, a narrowing of the spaces in your spine that puts pressure on your nerves. It can lead to calf muscle pain (and pain in the thighs, lower back, or buttocks) that worsens when standing or walking, but typically improves when you sit down or lean forward. Scientific research on neurogenic claudication provides further insight into this nerve-related issue.
- Arterial Claudication: Unlike neurogenic claudication, arterial claudication is caused by narrowing or blockages in the arteries that supply blood flow to the legs. This leads to cramping or pain in the calf (and other leg muscles) during physical activity like walking, which typically subsides with rest.
- Compartment Syndrome: This occurs when excess blood or fluid builds up underneath tough, inelastic tissues in the lower leg. This increased pressure can damage nerves and blood vessels, causing intense pain, swelling, numbness, and tingling. It can be acute (often due to trauma) or chronic/exertional (occurring during exercise).
- Varicose Veins: These are enlarged, twisted veins, often visible just under the skin. Damaged valves in these veins can lead to blood pooling, causing aching, throbbing, burning, swelling, and itching in the calves.
- Baker’s Cyst: A fluid-filled sac that forms behind the knee, sometimes rupturing and causing fluid to leak into the calf, mimicking a DVT with swelling and pain.
- Diabetic Neuropathy: Nerve damage related to diabetes can cause tingling, numbness, and burning pain that often radiates to the calves.
- Osteomyelitis: A rare but serious bone infection in the lower leg, which can cause redness, swelling, warmth, and pain in the calf, often accompanied by fever and fatigue.
Given the range of potential causes, a thorough evaluation is essential if your calf muscle pain is severe, persistent, or accompanied by any of the red flags mentioned.
Diagnosis and Treatment Pathways for Calf Muscle Pain
When calf muscle pain becomes more than a temporary nuisance, it’s time to seek professional guidance. Getting an accurate diagnosis is paramount to ensuring you receive the most effective treatment.
Getting a Proper Diagnosis
Our approach at Get Well Chiropractic in Northville, MI, always begins with a comprehensive understanding of your condition.
- Doctor’s Visit: We’ll start by discussing your medical history and the nature of your calf muscle pain. Be ready to describe:
- When the pain started and what you were doing.
- The exact location and intensity of the pain.
- What makes it better or worse.
- Any other symptoms you’re experiencing (numbness, tingling, swelling, fever, etc.).
- Physical Examination: A thorough physical exam will help us assess your range of motion, strength, flexibility, and identify any tenderness or swelling in your calf. We’ll check for signs of nerve involvement or vascular issues.
- Imaging Tests: Depending on the initial findings, we may recommend imaging tests to get a clearer picture of the underlying issue:
- Musculoskeletal Ultrasound: This non-invasive test can help us diagnose conditions like arterial claudication, Achilles tendinitis, or deep vein thrombosis (DVT). It’s also useful for assessing muscle strains and guiding injection therapies.
- MRI (Magnetic Resonance Imaging): For more complex cases or suspected severe tears, an MRI can provide detailed images of soft tissues, bones, and nerves.
Immediate At-Home Care: The RICE Method
For mild calf muscle pain due to strains or minor injuries, the RICE method (Rest, Ice, Compression, Elevation) is your go-to immediate treatment. We often recommend this approach for the first 24-72 hours.
- Rest: Stop any activity that causes or worsens the pain. Give your calf muscles a break to allow initial healing. Continuing to push through the pain can lead to further injury and prolong recovery.
- Ice: Apply an ice pack or cold compress to the injured area for 10-20 minutes every 1-2 hours for the first 3 days. This helps reduce swelling and inflammation. Always use a thin cloth between the ice and your skin to prevent ice burns.
- Compression: Gently wrap the lower leg with an elastic bandage or compression stocking. This helps reduce swelling and provides support. Ensure the bandage isn’t too tight, as it could cut off circulation (watch for numbness, tingling, or increased pain).
- Elevation: Whenever possible, prop up your injured leg on a pillow, keeping it liftd above the level of your heart. This assists gravity in reducing swelling.
In addition to RICE, over-the-counter pain medications like ibuprofen or acetaminophen can help manage discomfort. We also advise following the “No HARM” protocol for acute injuries: no Heat, Alcohol, Running, or Massage for the first 48-72 hours, as these can increase swelling and bleeding.
Professional and Advanced Treatments
If your calf muscle pain persists, is severe, or doesn’t respond to home care, we’re here to help. Our personalized approach at Get Well Chiropractic in Northville, MI, focuses on natural healing and long-term wellness.
- Physical Therapy: For muscle strains and Achilles tendinitis, physical therapy is often crucial. A physical therapist can guide you through specific exercises to restore strength, flexibility, and range of motion, ensuring a safe return to activity.
- Chiropractic Care: If your calf muscle pain stems from nerve impingement (like sciatica or neurogenic claudication) or biomechanical imbalances, chiropractic adjustments can be highly effective. We focus on addressing spinal misalignments and nerve interference that can radiate pain down to your calves. Our targeted chiropractic adjustments, combined with gentle therapies, aim to relieve pressure off the nervous system and promote proper body alignment.
- Massage Therapy: As part of a holistic treatment plan, therapeutic massage can be incredibly beneficial for releasing tight calf muscles, improving circulation, and reducing pain. It’s a wonderful complement to chiropractic care, helping to relax muscles and aid in recovery. Learn more about how we can help you take control of your recovery with massage therapy.
- Medications: Depending on the diagnosis, your doctor might prescribe muscle relaxants, stronger anti-inflammatory drugs, or other medications to manage pain and symptoms. For conditions like osteomyelitis, antibiotics would be necessary.
- Surgery: In rare cases, such as a complete muscle tear, severe compartment syndrome, or advanced spinal stenosis, surgery may be required to repair the injury or alleviate pressure on nerves.
Recovery Timelines for Calf Strains
The time it takes to recover from a calf strain varies significantly depending on its severity. We categorize strains into three grades:
| Strain Grade | Description | Typical Recovery Time (Rest) |
|---|---|---|
| Grade 1 (Mild) | A mild pull or slight overstretch of the muscle fibers. You might feel a strong pulling sensation. | 10 to 12 days |
| Grade 2 (Moderate) | A partial tear of the muscle fibers. You’ll likely experience sharp pain and difficulty walking. | 16 to 21 days |
| Grade 3 (Severe) | A complete rupture of the muscle. This causes severe pain, significant swelling, and inability to bear weight. | Up to 6 months (especially if surgery is involved) |
It’s important to allow your calf to heal fully before returning to full activity to prevent re-injury. Most people recover fully from pulled calf muscles without any permanent damage, but patience and adherence to your treatment plan are key.
Preventing Future Calf Pain: A Proactive Approach
Once you’ve experienced calf muscle pain, you likely want to avoid a repeat performance. The good news is that many instances of calf pain, especially those related to muscle strains and cramps, are preventable through proactive measures. By incorporating smart habits into your routine, you can keep your calves happy and healthy, allowing you to enjoy all the activities Northville, MI, has to offer.
The Importance of Warm-Ups and Cool-Downs
Think of your muscles like a rubber band: cold, they’re more likely to snap; warm, they’re pliable and resilient.
- Warm-ups: Before any physical activity, dedicate 5-10 minutes to a dynamic warm-up. This involves light cardio (like walking or gentle jogging) and dynamic stretches (leg swings, walking lunges). A proper warm-up increases blood flow to your muscles, improving their elasticity and preparing them for the demands of exercise. This is crucial for preventing sudden overstretching and strains.
- Cool-downs: After your workout, don’t just stop cold. Spend 5-10 minutes on a cool-down, including light activity followed by static stretching. Holding stretches for 20-30 seconds helps to improve flexibility and can aid in muscle recovery, reducing stiffness and soreness.
Strengthening and Flexibility Exercises
Strong and flexible calf muscles are less prone to injury. Incorporate these exercises into your routine:
- Calf Raises: Stand with the balls of your feet on a step (or flat ground). Slowly raise up onto your toes, holding briefly, then lower your heels below the step. This strengthens both the gastrocnemius and soleus.
- Gastrocnemius Stretch: Stand facing a wall, place your hands on it. Step one foot back, keeping your heel on the ground and your leg straight. Lean forward until you feel a stretch in your upper calf.
- Soleus Stretch: Similar to the gastrocnemius stretch, but with your back knee slightly bent. This targets the deeper soleus muscle.
- Foot Flexion: Sit on the floor with legs extended. Use a towel or resistance band around the ball of your foot and gently pull your toes towards your body, stretching the calf.
- Foam Rolling: Using a foam roller on your calves can help release muscle tension and improve flexibility.
Always perform stretches gently and avoid bouncing. If you’re recovering from an injury, consult with a healthcare professional before starting a new stretching routine to ensure it won’t aggravate your condition.
Lifestyle and Ergonomic Adjustments
Prevention extends beyond just exercise. Your daily habits also play a significant role:
- Proper Footwear: Wear supportive shoes that fit properly and are appropriate for your activity. Worn-out shoes can alter your biomechanics and increase strain on your calves.
- Hydration: Drink plenty of water throughout the day, especially before, during, and after physical activity. Staying well-hydrated is key to preventing muscle cramps.
- Nutrition: A balanced diet rich in essential minerals (like potassium, magnesium, and calcium) supports muscle function and can help prevent cramps.
- Avoiding Overtraining: Listen to your body. Gradually increase the intensity, duration, and frequency of your workouts. Don’t engage in activities you are not conditioned for.
- Gradual Progression: Whether you’re starting a new exercise program or returning after an injury, build up your activity level slowly. This allows your muscles to adapt and strengthen safely.
By adopting these proactive strategies, you can significantly reduce your risk of calf muscle pain and keep moving freely.
Conclusion: Take the Next Step Towards Pain-Free Movement
Calf muscle pain can be a real nuisance, impacting your ability to enjoy daily life and favorite activities. But as we’ve explored, understanding its causes, knowing when to seek help, and adopting preventive measures can empower you to regain control and move with confidence.
Here’s a quick recap of what we’ve learned:
- Understand the Cause: Calf pain can range from common muscle strains and cramps to more serious conditions like DVT, sciatica, or arterial claudication.
- Use RICE for Minor Injuries: For mild strains, the RICE (Rest, Ice, Compression, Elevation) method is your first line of defense.
- Know When to Seek Help: Always be aware of red flags like sudden, severe swelling in one leg, redness, warmth, or fever, which warrant immediate medical attention.
- Prevention is Key: Regular warm-ups, cool-downs, strengthening exercises, proper hydration, and appropriate footwear are vital for keeping your calves healthy.
At Get Well Chiropractic in Northville, MI, we believe in a personalized, natural approach to health and wellness. Whether your calf muscle pain stems from a muscle imbalance, nerve irritation, or simply needs some therapeutic relief, our expert team is here to help. We combine targeted chiropractic adjustments with gentle therapies and practical advice, focusing on natural healing and long-term well-being.
Don’t let calf pain cramp your style any longer. If you’re experiencing persistent or concerning calf muscle pain, we invite you to reach out. We’ll take your concerns seriously, perform a thorough evaluation, and help you get back to enjoying life to the fullest. Take control of your recovery with massage therapy and find how our comprehensive approach can make a difference.
